Managing Heel Pressure and How to Offload
What is Heel Pressure?

Heel pressure can cause serious injuries to the skin behind the heel and if not managed correctly can lead to further ulceration. This happens to people who have poor skin integrity or when people are not mobilising and are experiencing prolonged bed rest. The area behind the heel is prone to breaking down because the heel bone, called the Calcaneus, has a distinct ridge at the back of the heel that makes it prominent. The skin over the area is also thin and does not have much padding, such as muscle or fat that protects the bone from the skin.
Heel pressure occurs when people are laying down and the back of the heel is in contact with the bed. The weight of the leg is passed through the back of the heel where there is minimal padding or resilience to pressure. Movement of the heel on the bed will cause shear stress to the area and the skin can come red and inflamed.
Heel pressure areas are a common occurrence for a range of people. Most often people are experiencing long term bed rest when heel pressures occur. The skin protecting the area is thin and there is little tendon or muscle soft tissue protecting the bone. When people have poor skin integrity and are not mobilising often, they are likely spending a lot of time in bed. When you think about the position they are resting in, you notice their heels are resting right on the bed. Add micro-movements to this time laying down and the skin will experience ongoing shear pressure on the sheets or bed. This can cause pressure areas within hours; It may appear like a red blemish or when you wear a new pair of shoes and develop a heel blister. Or it may be a burst blister and forming into an ulcer.
Symptoms & Causes
As mentioned above, the pressure may first appear as discolouration on the heel, colours to look for are red, purple and blue. Like a bruise, the blood is at the surface of the skin causing the discolouration. It is likely that fluid will develop in the skin like a blister; once the skin breaks, the person is at risk of infection or skin death (necrosis).
There are several known factors that increase a patient’s risk of developing a heel pressure ulcer, including:
- Inadequate/malnutrition – Poor vitamin intake and absorption from food can lead to thinning of the skin and therefore decreased blood flow.
- Advancing Age – Elderly people who spend an increased amount of time in bed can lead to shear and pressure in areas of poor skin integrity.
- Abnormalities of circulation – This may be due to vascular issues where blood flow is limited to the extremities and a lack of red blood cells to an injury will delay healing. This is also common in patients with diabetes.
- Sensory deficiency – For example, people with diabetes who may experience nerve damage are at increased risk of pressure sores. Nerve damage causing loss of sensation is called Diabetic Neuropathy.
- Immobility – May be caused by paralysis, stroke or severe illness. Fractures of the bones in the legs may also lead to immobility for a period of time. Common fractures to occur are the neck of the femur (NOF) fractures also known as a broken hip
- Major surgery – Heart, lung and some orthopaedic surgeries restrict mobility and hence increase time in bed. Long periods of time laying in bed increase chances of pressure sores.
- Multiple health problems (comorbidities) – Particularly coronary or respiratory can lead to long term bed rest. Long periods laying in bed increases the chances of pressure sores.
- Dehydration – Hydration is vital for maintaining skin integrity and wound healing. Adequate fluid intake is necessary to support blood flow to wounded tissues and to prevent additional breakdown of the skin.
Treatment & Prevention
Offloading is described as lifting or pushing an area of high pressure away from the cause of the pressure. To offload is to distribute the load to other areas which are not susceptible to pressure areas. Both the calf and foot can help with the offloading. Heel pressure is redistributed to both the calf, a soft muscle belly which can change shape to fit a supportive device as well as the foot.
Below are some examples of devices available for short term or long-term offloading of the heel.
oapl Heel Cushion
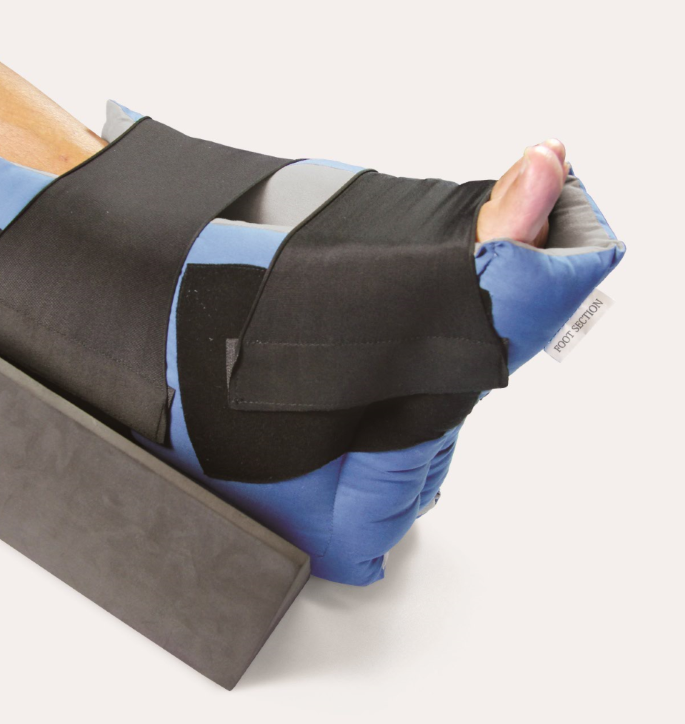
A basic all-rounder ankle, foot and heel relief device which acts as a snug cushion under the foot and ankle. A large hole under the heel allows for the pressure area to float in space and have minimal pressure in the heel region. The device is appropriate for prevention of pressures particularly in the ICU environment. The OAPL Heel cushion comes with a de-rotation wedge which limits rotation of the leg from the hip and keeps the leg in a neutral position. The device also comes with “AFO straps”, elastic straps which can be attached to the heel cushion (via Velcro) in a figure of 8 design, keeping the ankle at 90 degrees, avoiding plantar flexion and contractures occurring.
Heelift
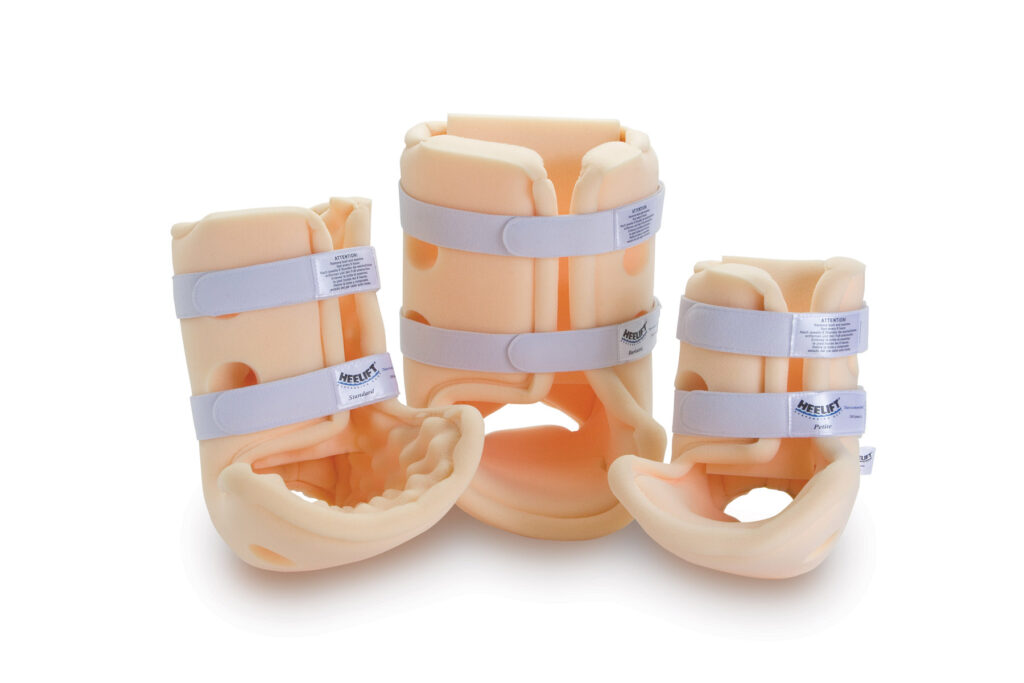
Available in smooth or convoluted foam. The Heelift Suspension Boot is designed to provide an effective solution for prevention and assistive healing of pressure ulcers at the heel. The Heelift delivers positioning and alignment of the lower limb. It is made from latex-free medical grade foam with a friction free tricot (satin) base. This ensures it stays in place on the leg at all times as well as sliding through the bed sheets when required and not sticking. The convoluted design is in place to aid air flow through the device when under the bed sheets. Heelift comes with an extra pad to control hip rotation, foot drop or provide added elevation. One size fits all.
MPO (Multi Podus Orthosis)

The RCAI MPO 2000® with Transfer Attachment features a Sky Blue breathable foam liner that wicks moisture away from the skin while maintaining skin integrity. The MPO floats the heel to eliminate pressure or friction on the heel, enhancing blood circulation vital to healing. The dynamic flex action supplies continuous counter force to the plantar surface of the foot assisting in the correction of foot drop, foot and ankle contractures and deformity. The adjustable toe post relieves pressure on the toes and can be positioned to the side in the treatment of malleolus and lateral ulcers. The rotator bar positioned to the side, controls hip and leg rotation, providing functional alignment. The transfer attachment (brown sole) is provided for stand-up transfer and prevents cross-contamination from floor to bed. We do not recommend patients walk in the MPO boot.